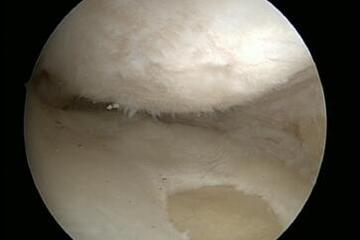
Cartilage damage
Unfortunately, cartilage injuries mostly affect young and active patients, so the demand on the therapy and the results are very high. However, the articular cartilage is not supplied with blood and has no nerve supply. It is nourished by diffusion from the synovial fluid and the adjacent bone. Therefore, cartilage injuries do not show a sufficient healing tendency, initial injuries can lead to joint wear. Surgical measures have a long post-treatment period, and often only a low load is allowed on the limb in order to achieve sufficient stability of the regeneration. Instabilities, axial defects, and ligament injuries of the knee joint must always be treated as well. Various therapy options are available to us for the treatment of cartilage injuries.
All therapy options have a specific field of application, and different risks and complications. Thus, the stage, size, and location of the cartilage injury determine the choice of procedure. Many of the procedures lead to the formation of so-called fibrocartilaginous replacement tissue rather than hyaline articular cartilage, but these therapies do show good medium-term clinical results. With bone-cartilage transplantation and cartilage cell cultivation, we also have procedures available that can lead to hyaline regeneration of the defect. So before the therapy, the damage must be diagnosed. Size and depth then determine the therapy. Simplified, this means that grade I/II damage is treated nonoperatively, i.e. conservatively, and grade III/IV damage is treated surgically. The size of the damage then comes into play in the choice of procedure. Damage <2.5 cm² is treated with microfracturing/nano drilling. In the case of very deep damage, a bone cartilage cylinder can also be used. Damage >2.5 cm² is treated with matrix-induced chondrogenesis or autologous chondrocyte transplantation. New procedures are constantly coming onto the market for the treatment of cartilage damage.